Healthcare Engineering
Numerical Simulation Research and Improvement of Surgical Procedures
The medical community is highly interested in improving the surgical protocol through reducing the surgery duration. This current study develops and validates a numerical Design-Structure-Matrix (DSM) simulation model of the entire laparoscopic cholecystectomy surgery structure, including coupling (loops) and rework.
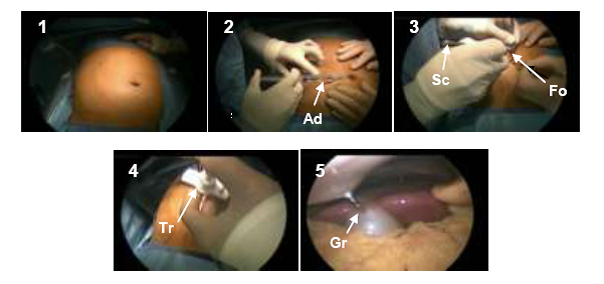
(a) Patient preparation. 1: Insufflations (A1). 2: Local anesthesia (A2). 3: Incisions (one infraumbilical plus three others) (A3). 4: Placement of trocars (A4). 5: Insert tools (e.g., grasper) posteriorly (A5).
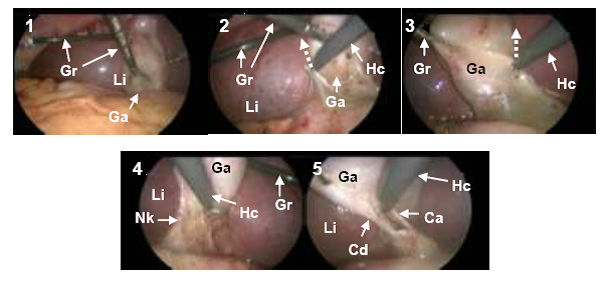
(b) Peritoneal preparation. 1: Expose the gallbladder with grasper (A6). 2: Dissect the left side of the gallbladder with hook cautery (A7, A8, A9, broken arrows indicating the direction of Hc motion). 3: Dissect the right side of the gallbladder with hook cautery (A10, A11, A12, broken arrows indicating the direction of Hc motion). 4: Dissect the back side of the gallbladder neck with hook cautery (A13, A14, A15, A16). 5: Expose the cystic duct and cystic artery (A17, A18).
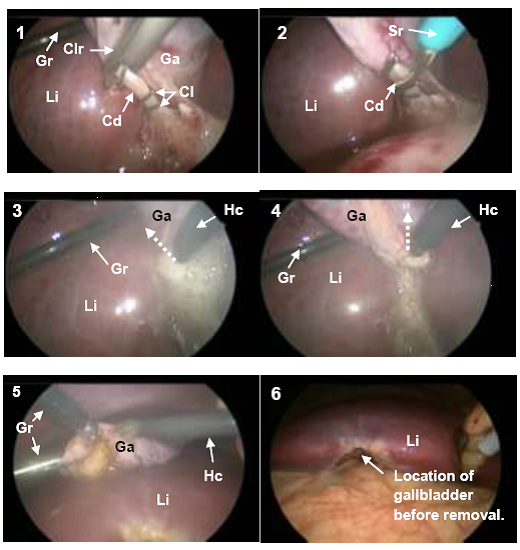
(c) Removal of gallbladder. 1: Clip the cystic duct and artery with a clipper (cystic artery not shown, located posterior to cystic duct) (A19, A20, A22, A23). 2: Cut the cystic duct and artery with hook scissors (A21, A24). 3: Separate gallbladder from liver on the left side (A25, A26, broken arrows indicating the direction of Hc motion). 4: Separate gallbladder from liver on the right side (A27, A28, broken arrows indicating the direction of Hc motion). 5: Mobilize the gallbladder (A29). 6: Clean/close (A30).
The figures above depict surgical activities involved in laparoscopic cholecystectomy.
(Ad: Anesthetic drug. Ca: Cystic artery. Cd: Cystic duct. Cl: Clip. Clr: Clipper.
Fo: Forceps. Ga: Gallbladder. Gr: Grasper. Hc: Hook cautery. Li: Liver. Nk: Neck.
Sp: Scalpel. Sr: Scissors. Tr: Trocar.)
The surgical activities above are analyzed through numerical Design Structure Matrix
simulation below, showing 5 coupled loops, 8 groups of conditional activities including
4 output parallel, and 4 input parallel groups.
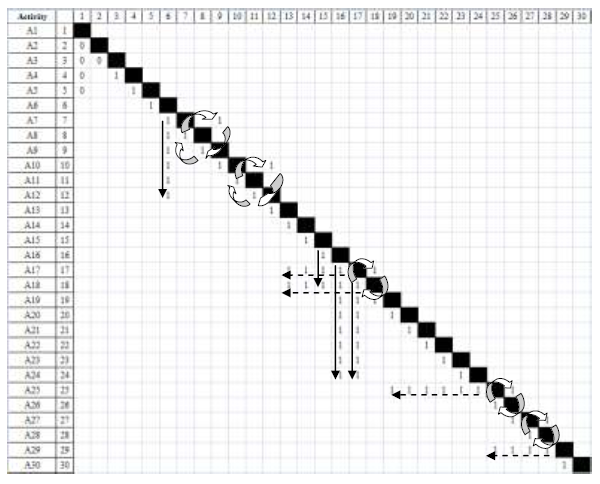
The model provides a framework that affords exploring the effects of alternative activities, testing redesign of the surgical procedure, and comparing different versions of surgical protocol through simulation.
Department of Mechanical Engineering
-
Address
Texas Tech University, Box 41021 | Lubbock, TX 79409 -
Phone
806.742.3563 -
Email
mechanical.engineering@ttu.edu
